Unfortunately, this question is often fuelled by fear and anxiety that has, in part, been created by the shocking amount of misinformation and extreme generalizations created by internet sites showing pictures of “worst-case scenarios.”
This 4-part blog series on lymphedema is designed to provide you with accurate knowledge about the lymph system and lymphedema. By the end of this series, you will be one step closer to knowing how to reduce your risk of developing lymphedema and how to detect it early.
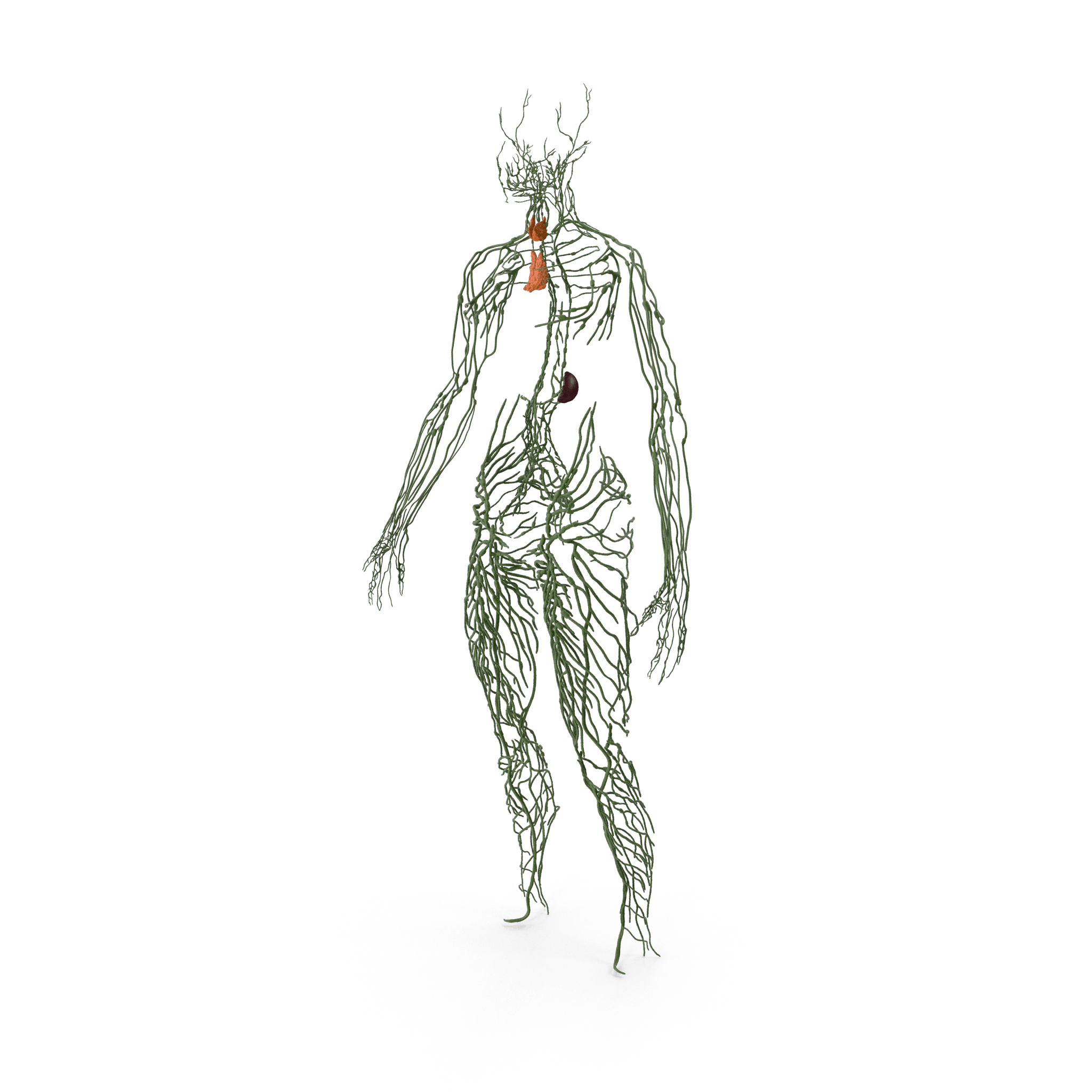
What is the Lymphatic System?
Our lymph system is designed to help our circulatory (blood) system remove fluid, proteins and waste products from our tissues and return them back to the heart. In addition, the lymph system has an immune function (i.e. fights bacteria and viruses) by producing and transporting immune cells.
Structurally, it is made up of lymph vessels, lymph nodes and lymphoid tissues. It contains both superficial and deep lymphatics:
- Superficial lymphatics:
- These consist of vessels located just below our skin, lymph nodes in our armpits (axillary nodes) and groin (inguinal nodes).
- Deep lymphatics:
- These consist of vessels located deeper in the body and lymph nodes in the pelvis, abdomen, neck (cervical) and above the collarbone (supraclavicular).
Watershed Lines
If we drew an imaginary line vertically and horizontally through our belly button (front and back), that would divide our torso into 4 quadrants. We call these lines “watershed lines”, because lymphatic fluid tends to move or drain away from these imaginary lines towards its nearest superficial lymph node bed.
For example, the lymph nodes in the left armpit will receive lymphatic fluid from the left arm and hand, as well as the left upper quadrant (front and back) of the body. This is very important to understand, as lymphedema risk (which we will discuss below) is NOT just about an arm or a leg.
So how does the System work?
Remember that part of the lymphatic system is made up of lymph vessels and lymph nodes. The lymph vessels’ job is to absorb fluid and proteins from the tissues and transport it (like a conveyor belt) back to the heart. On route, all lymphatic fluid will pass through its respective lymph node bed (remember what I mentioned earlier about watershed lines).
The job of the lymph nodes is to filter, clean and fight any potential infections in the lymphatic fluid. In other words, the lymph nodes are part of our immune system and are responsible for the start of an immune reaction if our body detects a threat.
After our lymph nodes have filtered the lymph fluid, most lymph will then enter the deep lymphatics and eventually find its way back up to the deep veins behind our collarbones (called the right and left subclavian veins), just before they enter the heart. This is the “drop-off” part of the lymphatic system.
Your next steps…
Click here for part 2 of this series: What is lymphedema?
Want to learn what YOU can do to reduce your lymphedema risk?
Disclaimer – These blogs are for general information purposes only. Medical information changes daily, so information contained within these blogs may become outdated over time. In addition, please be aware that the information contained in these blogs is not intended as a substitute for medical advice or treatment and you should always consult a licensed health care professional for advice specific to your treatment or condition. Any reliance you place on this information is therefore strictly at your own risk.